Doctors who treat life-threatening strokes by threading catheters and devices up from the groin into the brain have long believed they could save more lives if only they could safely grab hold of clots blocking large vessels and remove them. But the technology proved stubbornly difficult, and until recently it had not caught up with their hopes.
Now, finally, there is scientific evidence that clot retrieval can make a difference. A study published online this month in The New England Journal of Medicine reported that patients whose clots were extracted with an endovascular (in-the-artery) device had better outcomes than patients who were treated with medication alone. The study results, published by researchers in the Netherlands, were welcomed by two Mayfield Clinic specialists who perform endovascular surgery: Andrew Ringer, MD, a neurosurgeon, and Todd Abruzzo, MD, an interventional neuro-radiologist.
“For many years there have been a lot of stroke specialists who believe that doing something aggressive to remove the clot from the arteries inside the head could be an effective way to treat stroke, if we could just get there quickly and safely,” says Dr. Ringer, Professor of Neurosurgery at the University of Cincinnati College of Medicine. “The difficulty was having the technology to do it. Several years ago, that technology started to appear, but we still needed absolute scientific proof that it worked.”
The Dutch study “is the game changer we’ve been waiting for,” says Dr. Abruzzo, a Professor of Neurosurgery, Radiology, Biomedical Engineering, and Pediatrics at UC. “It’s what we have been trying to prove for years in Cincinnati.”
“For people who are at risk for stroke, this is great news,” Dr. Ringer adds. “We have a new and more effective way to treat it.”
Every year, about 630,000 Americans and 20.5 million people worldwide suffer an ischemic stroke, or “brain attack,” caused by a blood clot. In as many as half of those strokes, the clots are lodged in a large vessel. Because the large clots cannot be easily dissolved with the clot-busting drug tPA, patients who suffer such blockages are at grave risk of dying or suffering profound disability.
In February 2013, results of the earliest attempt to show that removing blood clots with a device could benefit patients at risk of stroke were published. The study, called the Interventional Management of Stroke III trial, showed that removing clots with a device did not help patients. But the study came with an unstated asterisk: “It was started before the technology had really matured,” Dr. Ringer says.
Now, less than two years later, the newer Dutch study, which used second-generation stent retrievers, has shown clear benefits to patients. The study, called MR CLEAN (Multicenter Randomized Clinical trial of Endovascular treatment for Acute ischemic stroke in the Netherlands), involved 500 patients who had suffered an acute ischemic stroke caused by a blockage of a large blood vessel. Of those patients, 90 percent were treated with the clot-dissolving drug tPA. Within that sub-group, 50 percent also received endovascular removal of the clot. Of those who received both tPA and endovascular treatment, 32.6 percent went on to live independently, compared to 19.1 percent of those treated with tPA alone.
As a result of the MR CLEAN results, two similar trials were stopped early because of benefits in the endovascular treatment group and a third trial was put on hold.
The technology used in MR CLEAN involved the Solitaire™ device, developed by Covidien, which looks like a stent but remains attached to a wire. The stent, which resembles a tube of chicken wire, is delivered up from a small incision in the groin through a catheter and deployed inside the offending blood clot. With the clot trapped inside the device, the physician pulls out the wire, retracting the wire, stent, and clot back down through the body and out the incision in the groin.
Even better news is likely to follow, as the “stentriever” techniques used in the Dutch study are already being displaced by even more effective methods. “Our stroke team is highly experienced with the modern technologies used in the Dutch study and is using even more advanced methods today,” Dr. Abruzzo says.
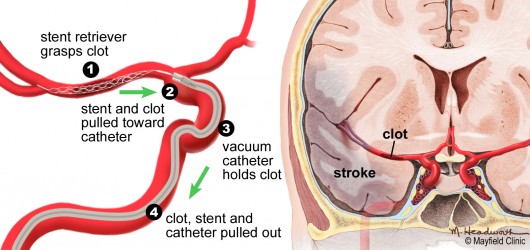
For a few years now Drs. Abruzzo and Ringer have been using two devices in tandem to achieve optimal results: 1) the Trevo® (manufactured by Stryker) or Solitaire™ stent retriever and 2) a vacuum catheter (the Penumbra System), designed to suck out the clot. “We deploy the stent retriever through the inside of one of these vacuum catheters,” Dr. Ringer explains. “And once we have the clot stuck in the stent retriever, we use the vacuum to help hold onto it so that we don’t lose any pieces of the clot as it is being pulled out.” Losing a piece of clot is potentially hazardous because a fragment could migrate through the blood vessels and cause a new blockage or stroke.
The Dutch study is the first of many studies to come that will demonstrate the effectiveness of interventional therapy, Dr. Abruzzo says. He and Dr. Ringer are involved in one of those studies at the Comprehensive Stroke Center at the UC Neuroscience Institute. The study is called THERAPY (Assess the Penumbra System in the Treatment of Acute Stroke).
— Cindy Starr